If your calf seizes up at night and you also notice bulging veins, you might wonder if the two are connected. These sudden, involuntary cramps can disrupt your sleep or stop you mid-workout.
In many cases, they’re more than just a nuisance. They can signal that your circulation isn’t moving blood efficiently back to your heart, leading to pressure buildup in the lower legs.
This guide explains how vein health and muscle cramps are connected, how to tell the difference between common causes, and when it may be time to seek medical evaluation. You’ll also find simple ways to manage discomfort and support circulation at home.
What is a True Leg Cramp? (And What It Isn’t)
Imagine waking up to your calf knotting into a hard, painful ball that forces you out of bed. This “charley horse” is a classic leg cramp: a sudden, involuntary muscle contraction. These spasms peak quickly and often leave the muscle sore for hours.
While they frequently strike at night, they also occur after intense exercise or long periods of standing on hard floors. Identifying a true cramp requires distinguishing it from other common types of leg discomfort:
- Delayed-Onset Muscle Soreness (DOMS): A dull, lingering ache appearing a day or two after activity. In contrast, a cramp is an acute, visible “knot” that happens instantly.
- Restless Legs Syndrome (RLS): A frustrating urge to move to stop a “crawling” sensation. A cramp is a physical locking of the muscle fibers.
If your primary struggle is waking up with cramps, recognizing these patterns is the first step toward relief. Now, let’s explore where varicose veins fit into this picture and where they do not.
Can Varicose Veins Cause Leg Cramps? The Connection Explained
Have you ever wondered why your leg cramps flare up specifically after a long day on your feet? While many people reach for a banana to fix a perceived potassium deficiency, the root cause is often your “plumbing” rather than your diet.
Yes, varicose veins and chronic venous insufficiency (CVI) can directly contribute to leg cramps by disrupting how your body manages fluid and metabolic waste.
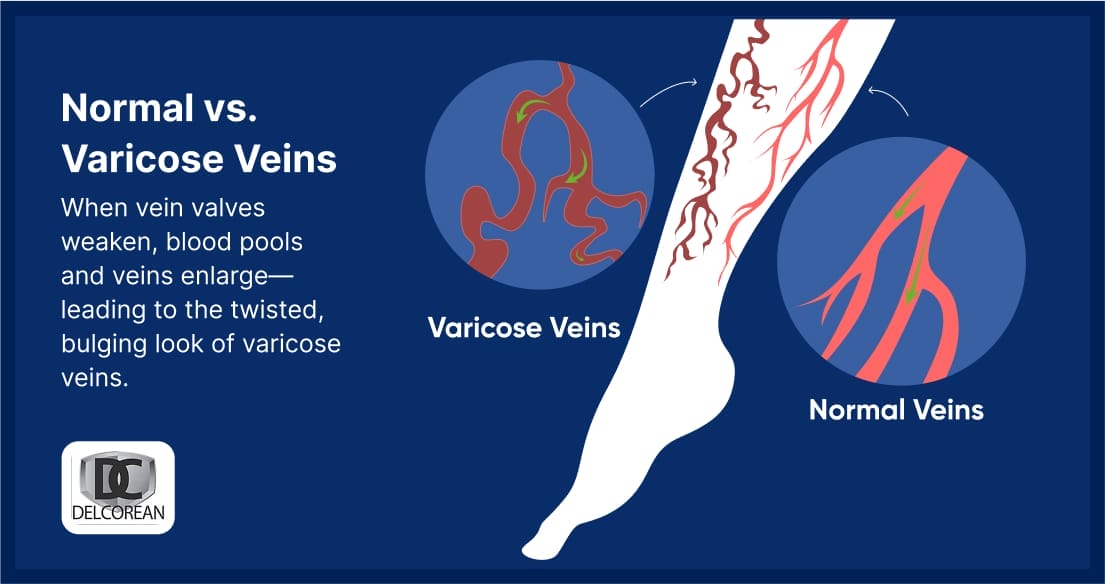
Healthy veins use one-way valves to fight gravity and push blood back toward the heart. When these valves fail, it triggers a specific four-step cycle:
- Valve Dysfunction: Weakened valves allow blood to leak backward, a condition known as reflux.
- Venous Stasis: Blood pools in the lower legs, particularly in the calves and ankles, instead of circulating efficiently.
- Pressure and Edema: Increased pressure inside the veins forces fluid into surrounding muscle tissue. This swelling stretches the skin and sensitive nerves.
- Tissue Irritation: This fluid buildup prevents fresh, oxygenated blood from reaching the area. The resulting accumulation of waste products irritates the local nerves, making the muscles hypersensitive and prone to involuntary spasms.
Your calf muscles act as a “second heart,” helping push blood upward when you move. Long periods of sitting or standing reduce this function, which is why vein-related cramps often appear at night or late in the day.
Common indicators of vein-related cramping include:
- Cramps combined with a “heavy” or aching sensation in the legs.
- Ankle swelling that disappears overnight.
- Itching, tingling, or “burning” sensations near visible veins.
- Symptoms that feel significantly worse after a long day of standing.
The tricky part is that dehydration, electrolytes, PAD, and RLS can feel similar. Here is how to sort through these causes to find the right treatment.

Decoding Your Leg Pain: Is It Varicose Veins or Something Else?
Cramps affect 60% of adults, and for 22 million Americans, these pains are tied to chronic venous insufficiency. While cramps are a nearly universal experience, the goal is not self-diagnosis: it is choosing the right next step for relief. Identifying specific symptoms helps determine if you are dealing with a simple electrolyte imbalance or a vascular concern.
Use this comparison to help categorize your discomfort:
| Trigger | Key Symptoms | Relief Factor |
| Vein-related (CVI) | Heaviness, swelling, or visible veins. Symptoms peak at the end of the day. | Better with elevation, compression, or movement. |
| Dehydration | Generalized cramps following heat, sweating, or illness. | Improves with water and electrolyte replacement. |
| PAD (Arterial) | Cramping pain during walking that improves quickly with rest. | Feet may feel cool or have reduced pulses. |
| Restless Legs (RLS) | Crawling or tingling sensations with an urge to move. | Relief comes with movement: not a hard “knot.” |
| Medications | Linked to statins, diuretics, or blood pressure meds. | Consult your prescriber: do not stop meds abruptly. |
When to Seek Emergency Care Today
Certain symptoms require an immediate visit to an emergency room or urgent care:
- Sudden one-leg swelling accompanied by warmth, redness, or severe tenderness (possible DVT).
- New shortness of breath or chest pain alongside leg symptoms.
- Fever paired with rapidly spreading redness on the skin.
- Sudden, severe pain in a foot that feels cold to the touch or looks pale.
When to Schedule a Routine Evaluation
If your symptoms are persistent but not an emergency, book a non-urgent appointment for:
- Recurrent night cramps paired with daily ankle swelling, heaviness, or visible veins.
- Skin discoloration around the ankles, itchy and dry skin, or sores that do not heal.
If you are not in the urgent category, you can begin managing symptoms and finding relief today.

Immediate Relief: How to Stop Leg Cramps and Support Your Veins
Imagine a sudden, searing knot in your calf bolts you awake, leaving you scrambling for the bed’s edge. While poor circulation often triggers these “charley horses,” you can regain control with these targeted steps.
Immediate Relief
- Stop and stretch: Pull your toes toward your shin to flex the calf muscle.
- Move: Walk for one minute or perform a light, gentle massage.
- Temperature: Apply warmth to relax fibers or cold if you notice inflammation.
Vein-Support Routine
- Ankle pumps: 2 sets of 20, 3x daily to improve circulation.
- Heel raises: 2 sets of 10 (use a counter for balance).
- Leg elevation: 10–20 minutes above heart level each evening.
Properly fitted compression socks also reduce the fluid buildup and spasms associated with vein issues. Additionally, audit dietary triggers like excess salt, sugar, or specific foods.
For fast relief during an active cramp, many people keep a topical roll-on from the Delcorean shop nearby. If cramps persist alongside visible swelling, here is what a professional evaluation involves.
Is Your Leg Cramp a Circulation Problem?
Determining if varicose veins cause your leg cramps requires looking at your symptoms as a whole. Because these cramps often stem from plumbing issues where poor venous return increases fluid pressure, rather than a simple mineral deficiency, your recovery plan must address both circulation and the muscle spasm itself.
Getting checked by a professional provides the clarity needed to choose the right treatment path without assuming you need a major procedure. Use this decision framework to determine your next step:
- Urgent Care Today: Seek immediate attention for sudden swelling in only one leg, redness, warmth, or accompanying chest pain and shortness of breath. These are critical red flags for a potential blood clot.
- Likely Vein-Related: Schedule a non-urgent evaluation if cramps are paired with visible bulging veins, a heavy feeling in the legs, or swelling that worsens after long periods of standing. Ask your clinician, “Should I get a venous duplex ultrasound to check for reflux and rule out a clot?”
- General Lifestyle Triggers: If cramps are tied to heat, dehydration, or intense exercise, start a 14-day conservative trial focusing on leg elevation and hydration.
If symptoms persist after two weeks, escalate your care. For those moments when a cramp catches you unprepared at night, keep a fast-acting topical like Cramp 911 from delcorean.com/shop/ on your nightstand. This allows you to manage the immediate pain while you work on your long-term circulatory health.
Frequently Asked Questions
Can varicose veins cause leg cramps at night?
Yes, varicose veins are a frequent cause of nighttime leg cramps because blood pools in the lower legs when the body is still. Without the “calf-pump” action of walking to move blood upward, pressure builds in the veins and irritates surrounding muscle nerves. This stagnation often leads to painful spasms shortly after you lie down to sleep or during periods of inactivity.
What are leg cramps, and are “charley horses” the same thing?
A charley horse is simply a common name for a sudden, involuntary muscle cramp, most often occurring in the calf or foot. These episodes involve a forceful contraction where the muscle fibers lock into a hard, visible knot. While the intense pain usually passes within a few minutes, the affected muscle may remain tender or sore for several hours afterward.
How can I tell the difference between restless legs and leg cramps?
Leg cramps are physical “knots” where the muscle visibly hardens and requires stretching to release, while Restless Legs Syndrome (RLS) is an overwhelming neurological urge to move. RLS typically feels like a crawling or tingling sensation that improves the moment you walk around. If these sensations frequently disrupt your sleep or make it impossible to rest, you should consult a specialist to rule out underlying vascular issues.
Do compression socks really help cramps caused by varicose veins?
Yes, compression socks help reduce vein-related cramps by applying graduated pressure that prevents blood from pooling in the lower legs. By supporting the vein walls, these stockings minimize the swelling and nerve irritation that trigger muscle spasms. For the best results, they should be worn during the day when you are standing or sitting for long periods to prevent evening fluid buildup.
Do certain foods like sugar or salt make leg cramps worse?
Excessive salt and sugar can worsen leg cramps by causing fluid retention and disrupting your body’s electrolyte balance. High sodium intake specifically increases swelling in the lower limbs, which puts additional pressure on veins already struggling with circulation. If dietary adjustments do not provide enough relief, many people use a targeted topical solution like Cramp 911 from Delcorean to address the localized muscle tightness immediately.
Note: Persistent, worsening, or one-sided swelling and pain should be evaluated by a clinician immediately.


